Pre-approval for nuclear imaging, cardiology, neurology, pain management and all surgical procedures.
How much time does your practice spend on pursuing in-house pre-approvals for nuclear imaging or other cardiology procedures? The pre-authorization process can be valuable for ensuring that a patient’s insurance will cover procedures, but on the other hand, it can be frustratingly time-consuming. Many physicians and administrative staff are finding that the lengthy process of pre-authorization cuts their productivity and turnaround times for care.
For many healthcare service providers, prior authorization can be a daunting task. In fact, medical prior authorization costs so much time and resources that it can offset some of the benefits of healthcare insurance on the part of service providers. Pre-authorizations can be time-consuming and expensive at the same time. Because of this administrative burden, many doctors and health care providers outsource necessary tasks to third-party medical billing service providers to cut operational costs and focus more time on providing better medical services. This article is meant to serve as your guide to understand everything you need to know, and if outsourcing is right for your medical office. First, let’s cover the basics:
What is pre-authorization?
Prior authorization refers to the process of managing the authorization or agreement given to the payer for approval about a medical billing service, procedural, or drug prescription. A payer may give its authorization for service and assign an authorization number that needs to be included on the claim during the submission for payment. In order to have a smooth flow in this process, ensuring the correct CPT code is needed. According to the American Medical Association: “Prior authorization (PA) is any process by which physicians and other health care providers must obtain advance approval from a health plan before a specific procedure, service, device, supply or medication is delivered to the patient to qualify for payment coverage. Other terms used by health plans for this process include “preauthorization,” “precertification,” “prior approval,” “prior notification,” “prospective review” and “prior review.”
Health plans often require this pre-authorization as a method for restricting access to costly services and therapies or checking that a proposed therapy is appropriate for the patient. The whole process can be disruptive and burdensome for physicians and their patients. Common issues include:
- Delayed access for patients to necessary services or therapies.
- Increased overheads for practices, especially where they need to hire staff to handle pre-authorization duties.
- Uncompensated time for physicians or other practice staff.
- Disruptions to and inefficiencies in the practice workflow.
The use of pre-authorization has been growing and is expected to continue doing so due to demand from health plans looking to lower or minimize costs. Many new therapies and treatments are coming out, but they are very expensive. While the current fee-for-service system remains in place, pre-authorizations will be an expectation.
Why is Prior Authorization Required?
There are several reasons a prior authorization is required. Every health insurance company uses a prior authorization requirement as a way to keep healthcare costs in check. This process will make sure that the service or drug that the physician is requesting is truly medically necessary. Requiring prior authorizations will also ensure that the service isn’t being duplicated. This is a concern when multiple specialists are involved with a single patient. And, this determines if an ongoing or recurrent service is actually helping the patient.
How much money does pre-authorization cost medical offices?
The AMA reports that pre-authorization consumes approximately 1 hour of physician time, 13.1 hours of nurse time, and 6.3 hours of clerical time per week. This translates to 853 hours per year of staff time, which is a cost of $82,975 in labor annually per full-time physician. A recent American Medical Association survey found that 90 percent of responding physicians believe that the “administrative burden related to PA requests has risen in the last five years, with most saying it has ‘increased significantly.’” As healthcare continues its acceleration toward value-based reimbursement models, payers may begin to require even more PAs as they seek greater cost controls.
According to the 2018 CAQH Index, an annual report on the adoption of electronic business transactions, 88 percent of PAs are submitted manually. For medical groups and practices seeking a more direct route to an optimized PA program, business process outsourcing (BPO) is proving to be a cost-effective and workflow-efficient solution to manually-driven authorization management.
How does outsourcing pre-authorization work?
Whenever you use an outsourced service for your pre-authorizations, third-party acts as a facilitator between your practice and the payer (such as insurance companies or Medicaid). The third-party company collects patient information from your practice to obtain prior authorization for inpatient and outpatient procedures, in addition to pre-certifications for hospital admissions. An advantage of an outsourced pre-authorization service is that they have developed a centralized and streamlined process that tends to minimize any patient data errors. They specialize specifically in this type of work so they are very familiar with the process and what needs to be done – unlike physicians and nurses who are trying to balance this with the rest of their work! An outsourcing company like Aqkode Healthcare Solutions will take care of tasks like:
- The end-to-end pre-authorization process
- Any follow-up that may be required, for example, if more information is needed from the physician for the pre-authorization.
- Appeals against denials where applicable.
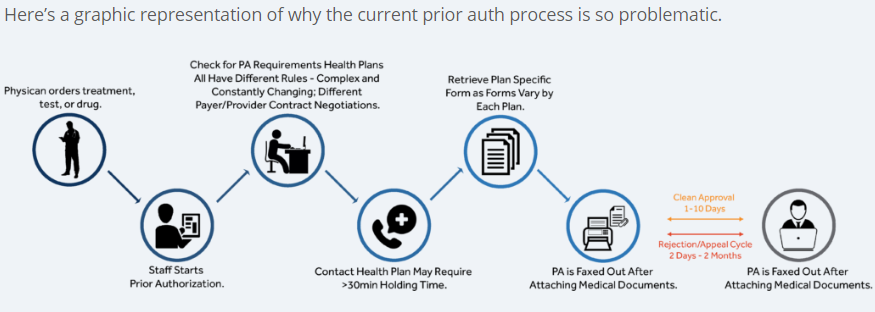

What are the benefits for doctors and physicians to outsource their pre-authorizations?
There are multiple benefits of outsourcing your pre-authorizations. The bottom line of whether it is the right choice for your practice is to look at the number of hours you are spending on pre-authorizations and what those hours are costing you. If outsourcing comes out on top with saving you time and money, then it’s probably the right move to make.
- Understanding payer-specific preauthorization requirements and monitoring for confirmation of payer decisions are activities that commonly suffer from a lack of consistency and slip-ups. They are often complex and inefficient for individual practices, which is where outsourcing comes in. Good third-party companies keep their team members up-to-date with training and compliance. They are dedicated to ensuring that those requests don’t slip through the cracks.
- Clearly defined roles and communication channels with physicians can also be an issue where practices (especially larger ones) handle their own pre-authorizations. Outsourcing mitigates these issues.
- Procedural issues are another common problem when it comes to pre-authorizations in practices. Procedures are often manual and cumbersome, involving binders of information and sticky notes. Adding to the complexity can be the need to figure out UMOs – third-party benefits providers used by the insurance companies. Outsourcing can mitigate these issues by centralizing procedures to a team with a good electronic process. Given that third parties do this all day, they have developed streamlined processes that help to get better results more quickly. They have efficiency and repeatability of processes on their side.
- Industry estimates put pre-authorizations at somewhere between $30 and $100 per occurrence. Staff members in practices spend up to nine hours each week just on hold for pre-authorization responses. Outsourcing is charged out in different ways depending on the company, but as a general rule, you can cut the cost of a pre-authorization right down. Many outsourced providers charge based on a per-study basis so even small clinics can leverage the service without worrying about minimums or expensive retainers.
Why choose Aqkode as your pre-authorization partner?
Outsourcing the prior authorization process allows you and your staff to spend more time on providing value and patient satisfaction. With Aqkode’s extensive industry experience and track record of timely service, your practice can enjoy on-time approvals while efficiently utilizing staff and management hours. This puts you in a better position to provide timely care and quality patient interaction.
Partner with Experienced Professionals. Prior authorization specialists are trained in the most efficient practices when it comes to handling your prior authorization requirements. They utilize the latest tools and technology platforms to help you streamline patient care while reducing the cost of conducting your practice. Prior authorization specialists are trained in the most efficient practices when it comes to handling your prior authorization requirements. They utilize the latest tools and technology platforms to help you streamline patient care and reduce the cost of conducting your practice. As a leading provider of pre-certifications for medical practices across the United States, Aqkode eliminates any administrative hassles when it comes to getting medical prior authorization approval. We custom-tailor our approaches for specific client needs while implementing a streamlined core process aimed to minimize data errors and ensure billing compliance.
Cut Expenses and Increase Revenue. Many organizations and private practices have experienced significant cost savings by outsourcing key administrative duties to third-party service providers. For many practices, cutting costs has been one of the biggest deciding factors when making a decision to outsource. Hiring a reputable prior authorization specialist allows you to leverage their proven, time-tested methods and tools to reduce operational costs, save practice money, and improve payment cycles and reimbursements. At Aqkode, we know how to keep costs down and pass those savings onto you.
Conclusion
The process of obtaining and maintaining prior authorizations is vital to the success of any medical practice. Overall, the prior authorization process impacts almost every aspect of the revenue cycle and operations of your medical practice. Resolve your administrative burden by partnering with a proficient prior authorization outsourcing company. Outsourcing your prior authorization needs will optimize your profit levels, improve claims processing, and increase on-time payments. At Aqkode Healthcare Solutions, we specialize in next-generation revenue cycle management, which includes prior authorizations, to help medical practices increase their cash flow and modernize their medical billing processes. To learn how we can help, schedule an appointment now.




